Understanding facial reconstruction
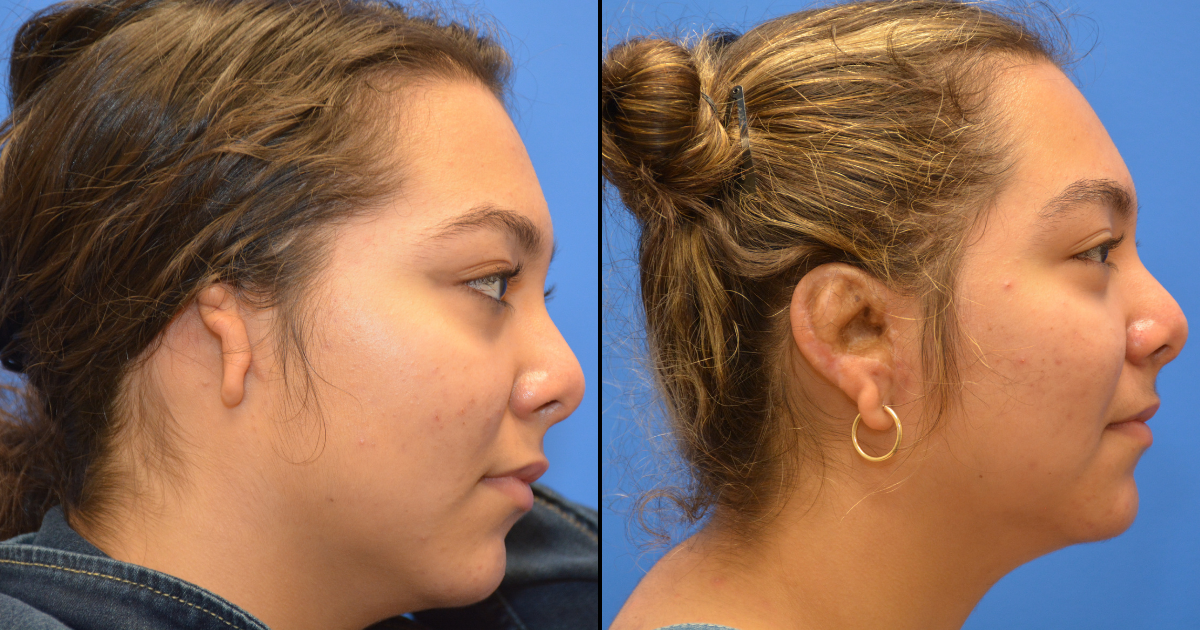
When people think of facial reconstruction, they often imagine cosmetic surgery or elective changes in appearance. In reality, reconstructive surgery is fundamentally different. Its goal is to restore the structure, function, and identity of the face.
Nebraska Medicine facial plastic and reconstruction surgeon Wes Heckman, MD, explains that facial reconstruction is about restoring what was lost.
“In simple terms, facial reconstruction is a surgery to restore someone’s normal form and function,” says Dr. Heckman. “Cosmetic surgery is typically done to enhance or improve appearance rather than restore it. However, when performing reconstructive facial surgery, it is critical to take aesthetic ideals into consideration to ensure an optimal surgical outcome.”
Facial reconstruction may follow cancer treatment, a traumatic injury or a condition present at birth. In many cases, it can help patients not only look like themselves again, but breathe, speak, eat and express emotion more naturally.
Why patients need facial reconstruction
The most common reasons for facial reconstruction fall into three categories.
Cancer
When skin cancer or other head and neck cancers are removed, they can leave behind significant defects.
“Ideally, we reconstruct the defect as soon as possible, often immediately after the cancer is removed,” says Dr. Heckman. “That allows us to restore both form and function in the same setting.”
Trauma
Car accidents, sports injuries, falls and other trauma can damage bones, nerves and soft tissue in the face.
“In traumatic cases, reconstruction usually happens within the first couple of weeks,” says Dr. Heckman. “Sometimes we need to wait for swelling to resolve before performing surgery.”
Congenital conditions
Some people are born with facial differences, such as a cleft lip, cleft palate, or congenital ear deformities.
“In certain congenital cases, surgery needs to be timed carefully,” says Dr. Heckman. “A child may need to grow more or be healthier before undergoing reconstruction.”

Why the face is so complex
Facial reconstruction can be challenging because the face is so visible and expressive in daily life.
“It’s not an area that’s easy to hide,” says Dr. Heckman. “The face is central to how we present ourselves and how we express emotions.”
Beyond appearance, the face is also responsible for essential functions such as, seeing, hearing, eating, speaking, and smelling. For example, patients with facial paralysis may struggle to move one side of their face which can impair how they protect their eyes, chew food, breath through their nose, or express appropriate emotions.
“When someone has facial paralysis, it affects movement, symmetry and even things like drooling or nasal breathing,” says Dr. Heckman. “Reconstruction improves both function and balance.”
Staged facial reconstruction
For complex cases, reconstruction may require multiple surgeries spread out over time.
“Staged surgeries are not uncommon, depending on the type of reconstruction we’re performing,” says Dr. Heckman. “That’s something we discuss with patients upfront.”
In some staged procedures, tissue may temporarily be positioned in a way that looks unusual while healing.
“Sometimes the tissue is in a temporary position that can appear just as noticeable as the original defect,” he explains. “It takes time and communication to help patients understand that it’s part of the process toward the final result.”
Recovery and long-term healing
Recovery varies based on the complexity of the procedure. Smaller reconstructions, such as scar revisions or minor skin cancer repairs, may only require a week or two of recovery. Recovery for larger surgeries may involve several weeks to months. Full healing may take longer.
“Tissue healing and scar maturation can take up to a year,” says Dr. Heckman. “We follow patients closely during that time to ensure they’re healing well and to determine whether any revisions or touch-ups might further improve their outcome.”
The emotional impact
Prior to reconstruction, many patients have already lived with a visible deformity or functional limitation.
“Some patients are hesitant to be out in public because of their injury or defect,” says Dr. Heckman.
When reconstruction restores a more natural appearance and improves function, the impact can be profound.
“It can significantly improve their quality of life and their confidence,” he says.
He recalls meaningful moments in his practice, including restoring a large portion of a patient’s nose after cancer removal to the point that most people couldn’t tell surgery had been performed. In another case, a patient with facial paralysis was able to smile again.
“Those are life-changing outcomes,” he says. “It’s incredibly rewarding to be part of that process.”
A collaborative approach to care
One of the many strengths of Nebraska Medicine is its team-based approach.
“We’re fortunate to have multiple specialists regionally with experience managing complex facial defects,” says Dr. Heckman.
Depending on the patient’s needs, care may involve plastic surgeons, head and neck surgeons and oral surgeons. When additional expertise is needed, specialists collaborate to create a comprehensive surgical plan.
“If we feel another specialist’s expertise would benefit the patient, we bring them in,” he says. “Working together ultimately leads to better outcomes and a better patient experience.”
Facial reconstruction restores identity, function and confidence. It helps patients move forward after cancer, trauma or congenital conditions with renewed comfort and self-assurance.





