A simple illness that turned into a crisis: How Nebraska Medicine supports patients living far from specialized care
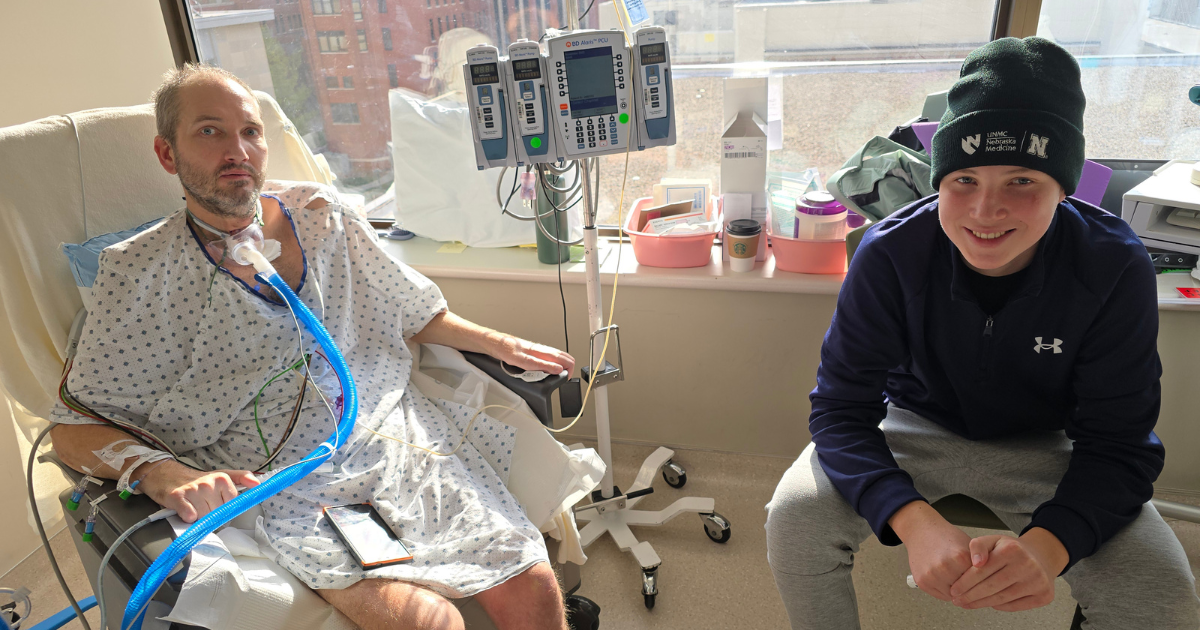
At first, it seemed like just a cold. For Mel Trumble and her husband, Tony, who lives with ALS, it quickly became something far more serious. What began as a routine illness in their hometown of Alliance, Nebraska, turned into a medical emergency that carried their family across the state and revealed both the strengths and challenges of receiving complex care in rural communities.
“Last Thanksgiving, he just woke up and couldn’t really breathe,” Mel recalled.
She rushed Tony to Box Butte General Hospital, where he spent the night in the Emergency Department. He was admitted the next morning, but it soon became clear he needed a higher level of care. On Nov. 30, Tony was transferred by air to Nebraska Medical Center in Omaha, where his ALS care team was based.
“It all happened so fast,” Mel said. “By the time they told me he had to be flown out, transport was already on the way.”
Tony required a breathing tube (intubation) for the flight. The next day, his breathing tube was removed, and he seemed to be improving. Initially, he was doing well, but a few days later, his oxygen level suddenly dropped dangerously low, and the breathing tube was reinserted (reintubated).
After that episode, the care team determined it was not safe to remove the breathing tube again. A tracheostomy became the safest option. Mel had never met otolaryngologist and head and neck surgeon Jayme Dowdall, MD, before that week, but she said Dr. Dowdall’s calm and clarity helped the family through one of the hardest decisions they would ever face.
“She was amazing,” Mel said. “She explained everything and made us feel comfortable that this was the right decision.”
Moving forward
Tony underwent tracheostomy surgery the Sunday after Thanksgiving. From that moment on, Mel says the Nebraska Medical Center team surrounded their family with compassion and support. Respiratory therapists began hands-on education immediately, helping Mel and her family learn how to care for Tony safely.
“The Neuro ICU was top-notch,” Mel said. “We cannot say enough about the care he received. The nurses and the RTs became like his family.”
The emotional toll of that week was heavy. On the day of surgery, the couple’s 14-year-old son, Emerson, saw his father with a tracheostomy for the first time and fainted in the hallway. Nurses quickly stepped in and caught him before he hit the floor.
After three weeks in the hospital, Tony’s condition stabilized, but the prolonged stay had taken a toll on his strength and worsened his ALS symptoms. Although the family hoped to be home by Christmas, it was not yet safe. Tony was discharged to Madonna Rehabilitation Hospital in Lincoln, where he received intensive therapy and made meaningful progress.
“They kept him busy from seven in the morning to 4:30 in the afternoon with PT, OT, speech and RT,” Mel said. “We saw a lot of progress.”
The goal then became returning home by New Year’s Eve. That transition brought a new challenge that underscored the difficulties faced by patients in rural Nebraska. The family encountered delays securing essential medical supplies and equipment needed to care for Tony safely at home. Despite repeated outreach by Nebraska Medicine, Madonna Rehabilitation Hospital and the family, options were limited.
Ultimately, Tony returned home on Jan. 8.
Outreach to rural providers
Knowing how isolated Mel and Tony felt, Dr. Dowdall followed through on a promise she made weeks earlier. She and nurse care coordinator Jade Rice traveled to Alliance on Feb. 14 to lead a hands-on tracheostomy training at Box Butte General Hospital.

The goal was simple: If a person with a tracheostomy arrived at the Emergency Department or if someone called 911, local health care professionals would have the training they needed to help.
Physicians, advanced practice providers, nurses, respiratory therapists and EMS personnel attended. Family members and friends also took part. Toni Girard, the sole respiratory therapist in Alliance, was there as well.
“She is here within five minutes if we need her,” Mel said. “Before this training, she was the only one who could help us.”
Since the event, the family says they feel more at ease.
“We feel way more comfortable now,” Mel said. “They know enough to help him and then get him where he needs to go.”
Extending education beyond Omaha
The training in Alliance reflects a broader effort by Nebraska Medicine and UNMC to extend education, resources and support beyond Omaha. Using funding from the Ambulatory Patient Education Fund, Dr. Dowdall and her team have developed realistic training models, hosted community education events across Nebraska and created instructional videos to support patients, families and health care workers.
Dr. Dowdall and team recently applied for the Rural Transformation Grant, which will provide funding to put systems in place to allow patients to get the care they need closer to home.
“We learned the need for resources in rural areas was greater than we could have imagined,” Dr. Dowdall said.
For the Trumble family, that commitment made it possible to return home safely.
“Thank you from the bottom of our hearts,” Mel said. “We may not have been able to say it to everyone who cared for Tony, but we hope they know how grateful we are.”





