What is thoracic outlet syndrome, and how is it treated?
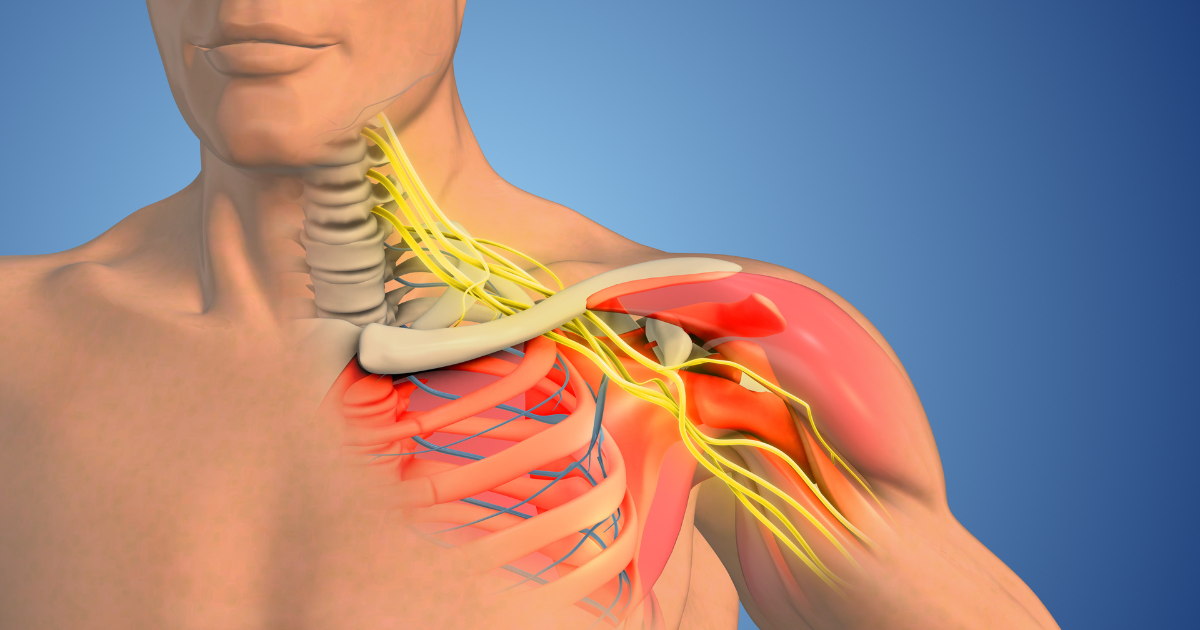
Important veins, arteries and nerves travel through a small space between your first rib and collarbone. This space is called the thoracic outlet.
Thoracic outlet syndrome (TOS) happens when the nerves or blood vessels in this space become compressed. Typically, this area is wide enough to allow the blood vessels and nerves to do their job. But sudden injuries, repetitive overuse or bone variations you’re born with can cause painful and debilitating symptoms.
Three types and their symptoms
Neurogenic (nTOS)
Neurogenic TOS happens when nerves are compressed, leading to ongoing pain in the neck, shoulder and upper back. Symptoms include numbness, pain, tingling and weakness in the arm and hand.
The most common type, nTOS often affects people in their 20s and 30s. Patients with Hypermobile Ehlers-Danlos Syndrome, a connective tissue disorder, are at higher risk.
Venous (vTOS)
Venous TOS happens when the subclavian vein is compressed, which affects the body’s ability to circulate blood through the arm. Symptoms include arm swelling or discoloration.
Venous TOS is usually diagnosed when a patient develops a blood clot in the axillary or subclavian vein, resulting in a deep vein thrombosis (DVT).
More common among younger people, it may be the first sign of an underlying blood-clotting disorder. It is also common among people who perform prolonged, repetitive overhead movements.
Young people on birth control who are diagnosed with DVT in the upper body will need screening for a blood-clotting disorder.
Arterial (aTOS)
Arterial TOS is the result of repeated injury to the mid-subclavian artery from a bony irregularity, such as an extra cervical rib or first rib defect. This results in a subclavian aneurysm. It often causes a loss of blood flow to the arm, leading to pain, numbness and discoloration of the hand.
More common in people in their 40s and 50s, arterial TOS can be limb-threatening, especially if left untreated.
How common is TOS?
Neurogenic TOS causes two to three cases per 100,000 people yearly. Venous TOS is less common, and arterial TOS is the rarest form.
Diagnosis
Diagnosis can be very complex and involve many factors. Conditions like carpal tunnel syndrome, neck pain from a cervical problem or back and shoulder pain must be ruled out before a diagnosis.
Unfortunately, young people are often underdiagnosed or misdiagnosed because symptoms can be vague or overlap with other conditions.
“While venous and arterial TOS are fairly straightforward, neurogenic TOS can be more complex,” says vascular surgeon Jason Cook, MD. “Young people, typically 16 years or older, with unexplained arm pain or abnormal blood clots should be evaluated. TOS is a diagnosis through a clinical suspicion after ruling out other problems, so getting the word out about TOS is really important.”
Testing may include:
- Electromyography (EMG), a nerve conduction study, to rule out peripheral nerve entrapment (as with carpal tunnel).
- Cervical spine MRI to evaluate the instability of the cervical spine.
- Shoulder evaluation by an orthopaedic specialist if injury is suspected.
- X-ray to check the cervical spine and look for a cervical rib. A cervical rib is an extra bone in the neck that some people have at birth, which can be removed.
Can TOS go away on its own?
“Neurogenic TOS can get better with physical therapy,” says Dr. Cook. “But venous or arterial TOS showing a clear rib abnormality will not get better on its own. It requires surgery to avoid long-term complications.”
Treatments for each type
Treatment depends on the type, but always aims to reduce symptoms and prevent complications. It’s essential to be your own advocate and seek out doctors with TOS expertise. A correct diagnosis is crucial before proceeding with surgery.
“Catching the condition early is key to determining the best course of action,” says Dr. Cook. “Long-term outcomes and quality of life are much better if we can diagnose and treat TOS before things get worse.”
Although TOS can occur on both sides at once, the worst side is treated first, then assessed again after recovery.
Neurogenic TOS
Treatment happens in stages:
- Stage one: Six to eight weeks of physical therapy.
- Stage two: An ultrasound-guided block (a lidocaine injection) is placed into the muscle. If symptoms improve, surgery is considered the next step.
- Stage three: Surgical decompression. If the block is positive and symptoms are disabling, the first rib is removed, and the scalene muscles are released.
Venous TOS
Early evaluation is crucial to prevent chronic swelling and improve long-term outcomes. To avoid lifelong blood thinners, surgery is typically needed.
Treatment involves:
- Medication, or a procedure called a thrombectomy, to remove the blood clot.
- Blood thinners for six weeks to allow inflammation to subside.
- Surgery to remove the first rib and release scar tissue around the vein.
- A bypass or patch is created to ensure ideal blood flow if compression continues.
Young patients with upper arm blood clots may be given anticoagulation treatment without a vTOS diagnosis.
Arterial TOS
A complex surgery is required to restore blood flow to the arm.
Surgery involves:
- Decompression, including removal of the first rib (and cervical rib if present) to address the aneurysm.
- A bypass graft to replace the artery.
Outcomes after treatment
Nearly all patients experience functional improvement with treatment.
“We’ve had particularly positive experiences helping young patients who were severely limited by their symptoms return to normal activities and quality of life after the procedure,” adds Dr. Cook. “We’ve treated over 75 people so far, with the majority experiencing major pain reduction, and no one has found their symptoms getting worse.”





