Using telemedicine technology to treat Ebola patients

Technology has always been my passion. I’ve spent several years at Nebraska Medicine in different areas of IT. One year ago, I started as telehealth coordinator and looked to continue my passion of identifying technology opportunities that benefit our physicians, nurses, staff and patients. The recent happenings with the Ebola virus have created opportunities for telehealth technology to improve patient care.
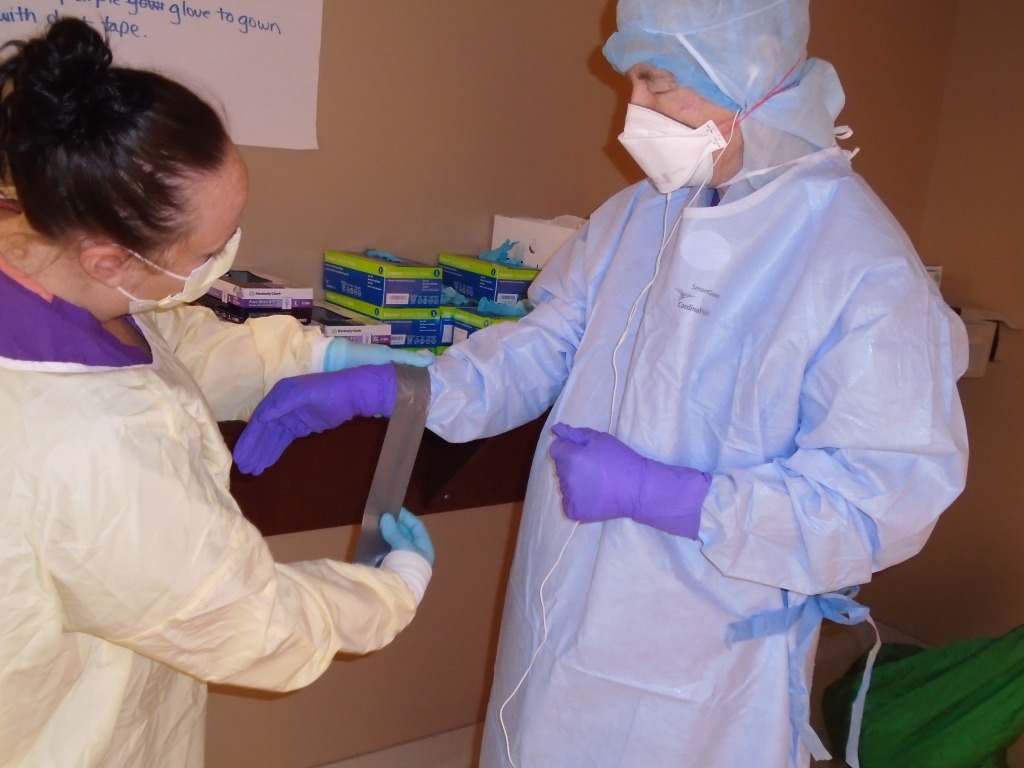
Operations inside our Biocontainment Unit run on incredibly strict guidelines. Infection control practices require 100 percent adherence. Personal protective equipment (PPE) and suits that use powered air purifying respirators (PAPR) can present unique communication challenges. All body parts must be shielded appropriately. Inside the patient’s room, your ears and mouth are covered and a full-face shield is worn. Team members go through a very important process called donning just to enter the patient’s room. Leaving the room involves an even more rigorous process called doffing. Simple tasks, such as listening to the patient’s heart and lungs become more difficult when you’re in PPE.
When treating Dr. Sacra, the staff initially used a Bluetooth stethoscope. But, the traditional ear pieces proved to be difficult while wearing PPE.
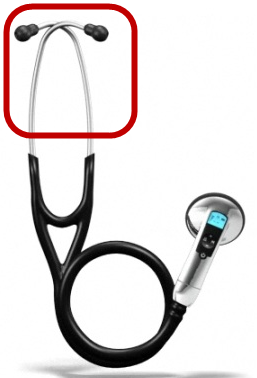
From the time our first Ebola patient, Dr. Rick Sacra arrived, I started working with Dr. Phil Smith, the medical director of the Biocontainment Unit, and lead nurse Kate Boulter, to identify new opportunities for telemedicine technology to help address some of these challenges. When treating Dr. Sacra, we initially started with a Bluetooth stethoscope that streams the sounds to another staff member located inside the unit. While the idea of streaming the sounds seemed helpful at first, the stethoscope still required the users to wear the traditional stethoscope ear pieces that fit down into the ear canal. The traditional stethoscope proved difficult for a number of reasons: staff would have to deal with the discomfort of trying to wear the stethoscope under their PPE; they would have to insert the earpieces into their ear canals on top of the protective hood; and the stethoscopes have limited lengths, which make it difficult to use with a full-face shield on. While the Bluetooth was helpful, it wasn’t our best option in the long run.
The ThinkLabs One stethoscope is placed on the patient, allowing staff to listen without having to bend down and get too close.
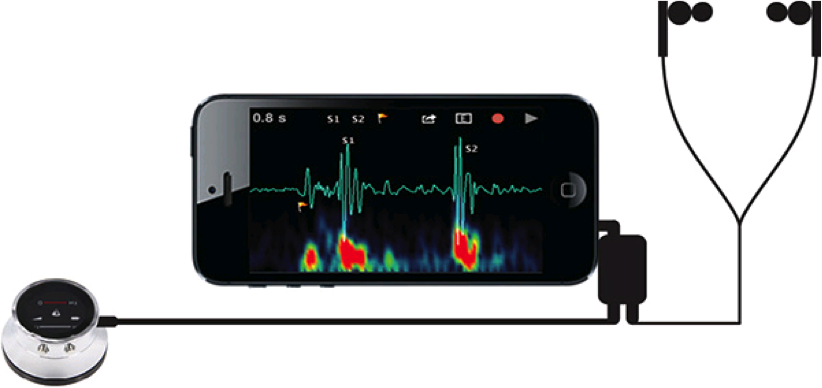
Before our second Ebola patient, Ashoka Mukpo arrived, I decided to try the new Thinklabs One electronic stethoscope. This stethoscope was invented from a new perspective. It becomes a transmitter of sounds. The user can listen to the sounds with earphones, use a mobile device to capture the sounds to be sent to medical staff, or do both simultaneously. Users of the stethoscope plug in headphones to an audio jack located within the device. They can adjust the volume and change the filter settings to target specific frequencies of sounds.

Electronic stethoscopes allow sounds to be transmitted to earphones, or captured with mobile devices to be shared with necessary providers. Staff can adjust volume and filter sounds accordingly.
The design of this stethoscope lends itself very well for the treatment of Ebola patients. I knew our team could place disposable earbuds under their protective gear, allowing the cord to be routed out of the suit to plug into the stethoscope, letting them hear what they needed without the risk of breaking safety protocol. Once they were done using the stethoscope, they could simply unplug their earbuds and dispose of them when they removed their PPE. The stethoscope could then be sterilized appropriately with bleach. Upon hearing this idea, workstation support quickly provided a box of iPhone earbuds for the Biocontainment Unit.
Once Dr. Smith has his personal protective equipment (PPE) on, he’ll enter the patient’s room and plug the earbuds into the Thinklabs One stethoscope.
When I met with Dr. Smith to demonstrate the Thinklabs One stethoscope, he was very excited about how well it worked. Dr. Smith was able to don a protective cap, put earbuds on over the cap and still hear the sounds loud and clear. The stethoscope and earbuds worked perfectly.
When Dr. Smith is done seeing the patient, he’ll dispose of the earbuds with the rest of his PPE. The stethoscope is sterilized appropriately using bleach.
On October 6, the day Ashoka arrived, the Thinklabs One stethoscope was used for the first time at Nebraska Medicine. The staff was ecstatic about how well it worked. These stethoscopes have quickly become a very important piece of technology in the treatment of infectious diseases. Nebraska Medicine continues to lead the way in setting the standard of care. Several other health care organizations are already inquiring about our use of this technology. Good news travels fast. Based off the effectiveness at Nebraska Medicine, the Thinklabs One stethoscope is currently being used to treat infectious diseases at a New York hospital.
Staff are able to wear disposable earbuds over their surgical caps, eliminating ear canal exposure.
With the successful treatment and discharge of two Ebola patients at Nebraska Medicine, we are now focused on education. We’re busy putting together documentation to share with other organizations and communities. Working with the Biocontainment Unit team and helping contribute to patient care has been an incredible learning experience for me. It’s extremely rewarding.
To learn more about the telemedicine technology being used inside the Biocontainment Unit, including videoconferencing and wireless X-rays, read this article in National Geographic.


