Using AI for immediate, on-site detection of diabetic retinopathy
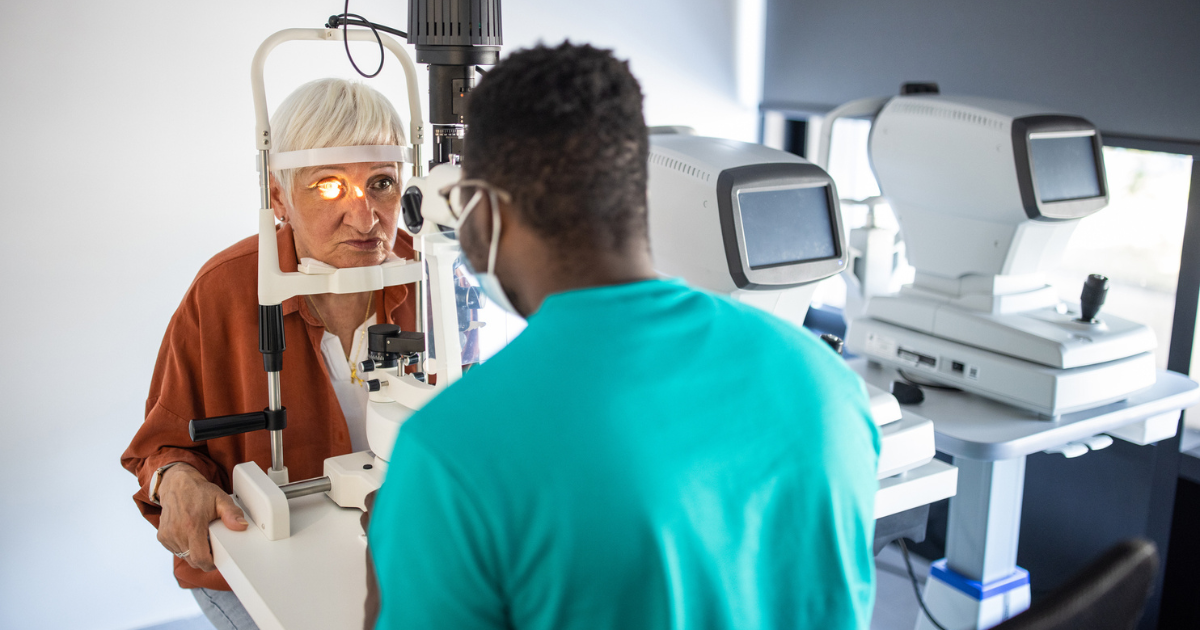
Artificial intelligence, or AI, is increasingly transforming many aspects of patient care, including in ophthalmology and primary care settings.
Nebraska Medicine launched EyeArt® in its family medicine clinics last month. EyeArt® is the first and only FDA-cleared AI technology for autonomous detection of vision-threatening diabetic retinopathy caused by high blood sugar.
It’s estimated that 40% of people with diabetes over age 40 will develop diabetic retinopathy, and 20% of those people will experience threats to their vision. You are at increased risk the longer you’ve had diabetes and the higher your A1C levels.
EyeArt® allows doctors to capture images of their patients’ retinas using a fundus camera that photographs the back of the eye. These images are securely transmitted to the system’s cloud-based platform, which looks for signs of disease or lesions and then returns a report in under 60 seconds. It may also detect age-related macular degeneration and glaucoma. However, it’s not intended to replace a complete eye exam, which can identify other things, such as the need for glasses.
EyeArt® is currently available at the family medicine clinics at Bellevue Health Center and Durham Outpatient Center. There are plans to expand across other clinics later this year.
If you are at least 22 years old and have diabetes, we encourage you to discuss EyeArt® with your doctor. Patients who receive a “normal” EyeArt® vision report will be cleared for another year. Anyone identified as having a potential risk for vision loss will be referred to an ophthalmologist or eye doctor.
“Because diabetic retinopathy often has no symptoms in the early stages, it’s important for patients with diabetes to have their eyes screened regularly,” says board-certified ophthalmologist Steven Yeh, MD. “Early detection and timely intervention can reduce the risk of vision loss and are essential, given that late-stage disease can be more difficult to treat.”
According to the company’s website, EyeArt® has been tested on over half a million patients globally, with over 2 million images collected in real-world clinical settings. EyeArt® reports a 91.3% sensitivity for referable diabetic retinopathy and a 98.5% sensitivity for vision-threatening diabetic retinopathy in a study of over 100,000 consecutive patient visits to over 400 primary care clinics.
“In many ways, the use of AI in health care is still in its infancy,” says Jeffrey Harrison, MD, chair of the Department of Family Medicine at UNMC. “This is one of the first introductions of AI as a diagnostic tool to improve patient care, and we’re excited to use it to better serve patients coming in for routine diabetic checks.”
Contact your doctor or diabetes care team immediately if you experience:
- Gradually worsening vision
- Sudden vision loss
- Floaters or shapes floating in your field of vision
- Blurred or patchy vision
- Eye pain or redness







