Autoimmune and blistering diseases: What to know about bullous pemphigoid, pemphigus and mucous membrane pemphigoid
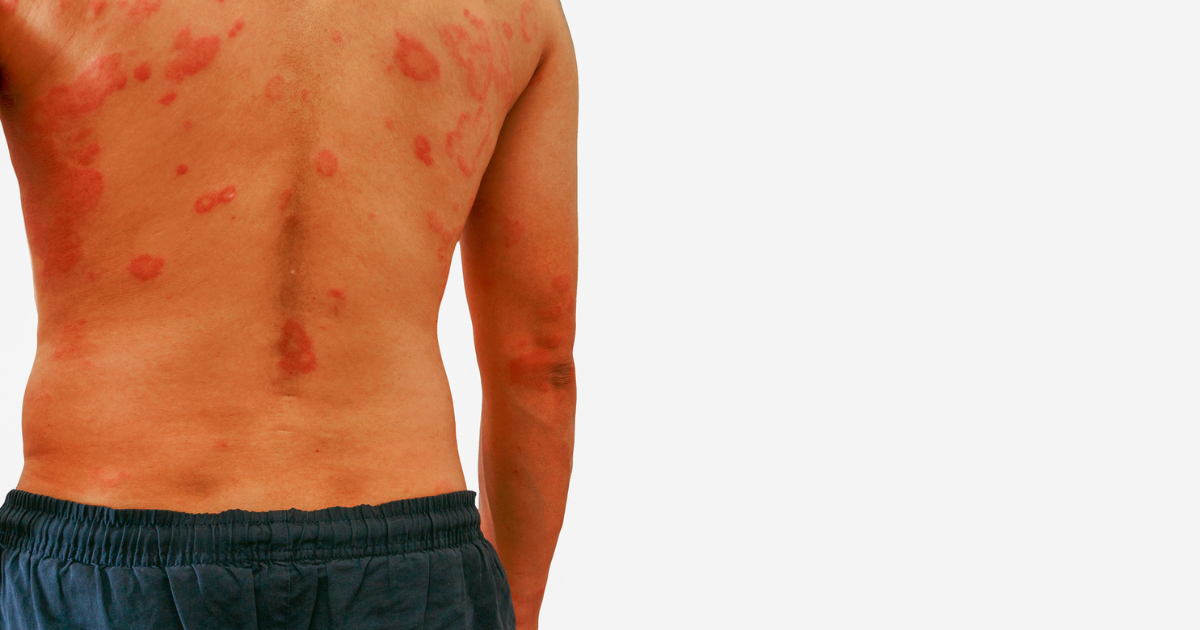
Autoimmune blistering skin diseases, although uncommon, can cause significant discomfort and can be life-threatening if left untreated.
Also known as autoimmune bullous disorders, these long-term conditions can cause severe itching, pain and disability. Causing the body’s immune system to mistakenly attack healthy skin tissue, they can result in blistering lesions that primarily affect the skin and mucous membranes, such as the mouth, eyes and nose.
Autoimmune blistering skin disorders are not contagious. While there is no cure, doctors can provide treatments to help heal the blisters and control the disease into remission.
Autoimmune blistering disease clinic
As the only clinic of its kind in Nebraska, this specialty clinic provides dedicated treatment and lifelong management for these skin condition types.
Dermatologist Corey Georgesen, MD, directs the clinic and uses the most current therapies to achieve the best outcomes. In addition to his dermatology expertise, Dr. Georgesen is also a trained dermatopathologist, giving him unique insight into the diagnosis of complex skin diseases.
“Autoimmune blistering skin diseases can come on suddenly, spread quickly and can be complex to treat,” says Dr. Georgesen. “If not treated effectively and promptly, they can lead to infections and other complications that may require hospitalization.”
Many of these diseases are lifelong conditions. Advanced diagnostic techniques provide a more accurate and definitive diagnosis. The goal of the clinic is to achieve long-term remission and gradually reduce a patient’s dependence on immunosuppressive drugs.
Streamlined, integrated care offers patients swift referrals to other physician partners in ear, nose and throat, ophthalmology, oral surgery, nutrition and other specialty areas.
The most common conditions treated at the clinic include:
- Bullous pemphigoid.
- Pemphigus.
- Mucous membrane pemphigoid.
- Epidermolysis bullosa.
- Hailey-Hailey disease.
- Porphyria cutanea tarda.
- Linear IgA disease.
- Dermatitis herpetiformis.
Patients also have access to clinical trials, which offer the opportunity to try advanced therapies not yet available to the general public.
What causes autoimmune blistering diseases
Although these skin conditions occur when the immune system incorrectly attacks the skin, doctors don’t know exactly why these diseases develop.
Normally, the immune system makes proteins called antibodies that attack bacteria and other foreign invaders that might make you sick. In these disorders, the immune system produces proteins that attack the substances that would normally bind the inner and outer layers of the skin together. This separates the two layers and allows fluid to collect, leading to blister formation.
Risk factors
Some people have genes that increase their risk of developing these disorders. In other cases, it may be triggered by certain blood pressure medications, antibiotics and specific cancer treatments.
Bullous pemphigoid
Bullous pemphigoid is the most common autoimmune blistering disease, especially among older adults, often between ages 60 and 80. Fewer than 20,000 people are diagnosed yearly in the United States.
Symptoms:
- Itchy skin that may develop weeks or months before blisters form.
- Large, hard, fluid-filled blisters along the creases or folds in the skin are often located in the abdomen, upper thighs or armpits.
- Red or dark colored skin around the blisters.
- Small blisters in the mouth or other mucous membranes.
For some, the blisters will go away on their own in a few months. But for other patients, it may take five years or more. Treatment usually involves anti-inflammatories and immunosuppression drugs that put the disease into remission.
Pemphigus
There are two types of pemphigus: pemphigus vulgaris and pemphigus foliaceus.
- Pemphigus vulgaris is more common in the United States and occurs most often in midlife or later.
- Pemphigus foliaceus is more common in Brazil and some areas of South America due to genetic and environmental factors, and in regions such as Turkey and North Africa.
Symptoms:
- Blistering, crusted sores that begin in the mouth and spread to the skin and genitals.
- Painful blisters that don’t itch.
- Sudden outbreaks of blisters or sores.
These sores are sometimes mistaken for herpes. The disorder can be fatal if left untreated.
Risk factors:
- Jewish ancestry, particularly Ashkenazi.
- Descendants from certain regions in Europe and Asia.
Pemphigus is typically a lifelong condition that can go into long-term remission with proper treatment. Current treatment may include immunosuppressive and immunomodulatory medications. Immunosuppressive drugs reduce the strength of the body’s immune system, while immunomodulatory drugs target certain pathways to turn down the proteins that attack the skin.
Mucous membrane pemphigoid
Mucous membrane pemphigoid is one of the rarest, chronic immunosuppressive blistering skin conditions.
“Mucous membrane pemphigoid is a potentially devastating disease that can result in permanent disability,” says Dr. Georgesen. “Early recognition and treatment are paramount. Patients with features of this disease should be referred to a board-certified dermatologist for diagnosis.”
Primary symptoms:
- Blisters, ulcers and scarring that affect the eyes, mouth, nose, genitals and other mucous membranes.
- Blisters, ulcers, pain and inflammation of the gums (gingivitis).
- Infection.
- Severe cases can cause scarring, difficulty swallowing and blindness.
Treatment consists of a combination of immunosuppressants aimed at quickly getting active inflammation under control and transitioning to long-term treatment that is safe and effective.
“Treatment with long-term immunosuppression puts these patients at risk for infection; therefore, coordination with a specialized care team to avoid complications is recommended,” adds Dr. Georgesen. “And while the goal of treatment is to induce remission, meaning a temporary recovery, there is potential for long-term relapse. This underscores the importance of establishing a relationship with a long-term care provider comfortable with treating and managing the disease for a lifetime.”
Learn more about the extensive services that Nebraska Medicine dermatology experts provide, including several subspecialty and multidisciplinary clinics.
Call 800.922.0000 or schedule an appointment online with one of our skin specialists.





